Msc Global Healthcare Management 7056soh Assignment Sample
Introduction
South Africa is going through one of the largest and most visible HIV epidemics in the world. Statistically, approximately 7.71 million women were living with the most dangerous disease HIV during 2018. South Africa is blameworthy for around majority of all the fresh HIV cases inside this region. In 2018, 2.5 million new coming HIV infections occurred, while 72,000 South African people resulted in death of AIDS-related diseases. World’s largest antiviral treatment (ART) program was introduced in South Africa. The chief funding of this program was assembled by domestic savings: in 2017, the nation spent upwards of $1.54 billion per year to conduct its HIV programs. South Africa’s Academic program has been a success, as indicated by the increase in nationwide mortality rate from “56 percent” in the year 2010 to “63 years”, recently in 2018.
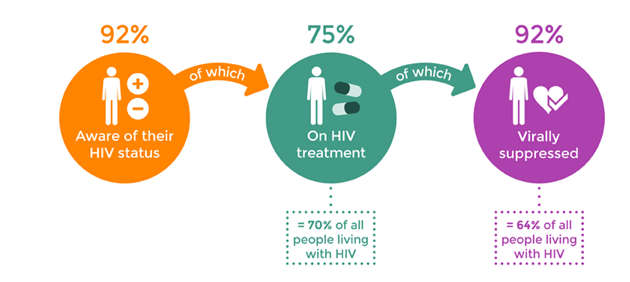
Figure 1: 90-90-90- Target for all age
(Source: www.avert.org)
South Africa is designing an important performance approaching the United Nations program on HIV 90-90-90 Targets, notably in terms of viral suppression as well as testing. In 2018, 90 percent of HIV-positive persons were able to cope with change, with “68 percent” receiving treatment. 87 percent of individuals identified and acquiring therapy were suppressed. This amounts to 62 % of all the patients infected with HIV, who reside in South Africa, are on medication, and almost 54 % are being dangerously subdued.
HIV prevalence is more with 20.4 percent of the entire population infected. The prevalence, unfortunately, varies widely by area, reaching from 12.6 % in the North West province to 27 % in KwaZulu-Natal.
Adolescent girls and young women
The incidence of HIV among young females is roughly fourfold of adolescent boys. In the year 2018, 540,000 young females, as well as 180,000 young people, were treated.
In that period, 69,000 girls and females were HIV-positive, compared to 28,000 young males, conveying those teenage girls are substantially more likely than young men to get HIV (Amuche et al. 2017). The disparity is most pronounced among adolescents aged 10 to 19, having 33,000 young women acquiring Disease in the year 2018, comparable to 4,200 teenage boys.
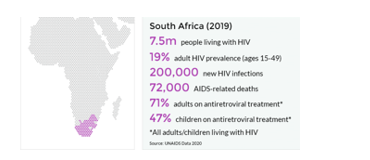
Figure 2: UNAIDS Data, 2020
(Source: Provided)
Intergenerational partnerships among older males, a demographic with a substantial HIV incidence, and inexperienced women were found to be the source of the transmission cycle (Chisale 2018). The Medium-Term strategic HIV Framework has focused its HIV preventive efforts on breaking this loop.
In the year 2016, the authorities began a national program to enhance the health of girls and women. This same She Conquers promotion aimed to reduce adolescent pregnancy, eliminate sexual identity violence, retain students in class, and expand economic prospects for girls and women (De et al. 2018). From before the prophylactic is now available for young ladies and teenage girls who’ve been regarded to be at high risk of contracting the disease (PrEP).
South Africa’s HIV testing and counselling (HTC)
In current years, South Africa undergone noticeable success within increasing the value of persons who get affected and tested for HIV. South Africa achieved another one of the 90-90-90 Target in 2017, with 90 percent of HIV-positive persons informed of their disease, up from 85 percent in 2015 (Dreyer, 2018).
This advancement comes after the introduction of two state-wide examining approaches: the health Promotion testing and consultation (HTC) candidacy in 2010 and indeed the HTC urban regeneration plan in the year 2013, both of those concentrate on persuading individuals to screen from either the business sector, farmland, and college education (Du et al. 2018). Every year, over 10 million South Africans test positive for HIV as a result of efforts like this.
However, progress in persuading individuals to test seems to have been unequal. Within South Africa, people seem far more probable than males to test. The reason behind this may be PMTCT interventions that allow women to have HIV laboratory testing.
Moreover, a recent guidebook has exposed those people who generally see the health care facilities as spaces for women, and hence believe that HIV testing is feminine. Men also expressed concern that collecting out the front of the testing centre may be interpreted as proof that they have HIV, and they discuss delaying testing even though they are absolutely petrified of a satisfactory outcome (Hihorst et al. 2018). As a consequence of the gender inequality in treatment, “93 percent” of Disease women became able to cope with change in 2018, compared to “88 percent” of HIV-positive males.
It has been determined by several researchers that in South Africa socio-economic factors are related to the high possibility of being tested positive for HIV for most people. Someone who has had an HIV test or knows their situation is much more likely to have a significant degree of training, to somehow be educated, to have correct HIV information, and also have an increased risk perception.
Although HIV testing rates have increased by province, extending to 82 % for bridging the gap to 88.3 % in KwaZulu-Natal, the people from the rural regions are up to three substantially less likely to have already been diagnosed with HIV than just those living in metropolitan areas (Huysamen & Boonzaier, 2018). The government NSP has highlighted fixing these inadequacies as either a primary concern, and it intends to decentralize testing because more businesses and communal venues may offer HIV tests.
South Africa is likewise increasing the use of self-examining. According to preliminary findings, 88 percent of persons who decline the standard process for testing embrace the opportunity of HIV consciousness (Jefferis & Theron, 2017). Consciousness has been proven to be a preferential testing option particularly for younger individuals and persons from important impacted social groups, including males who seem to have sexual relationships, according to a growing body of research.
South Africa’s HIV prevention programs
By 2022, South Africa hopes to lower the yearly figure of new cases to less than 100,00.
The authorities have intentions to do this through escalating preventive steps within the parliamentary constituencies which alone account for approximately “82 percent” of all HIV patients and the bulk of diarrheal diseases. It has also guaranteed to wipe out new diseases caused by women transmitting by 2022 (Karim et al. 2017). Furthermore, the x Government of South Africa LGBTQIA HIV Framework 2017 to 2022 promises to target 95 % of the LGBTI population with HIV / aids protection including ensuring 90 percent of LGBTI persons affected with HIV are able to cope with change.
A variety of HIV preventive initiatives being undertaken within South Africa in order to meet those aims are given as follows:
Prevention of mother-to-child transmission (PMTCT)
South Africa achieved remarkable success in lowering grandparent Spread of the virus since the past decade, having primarily led to advances within the accessibility of therapeutic interventions and the general availability of its preventive measures of grandparent transmission (PMTCT) initiative. In 2017, the frequency of caregiver transmission was 1.3 percent less than 3.6 percent in the year 2011.
In the year 2018, around 88 percent of expectant females have been infected with The virus, and 87 percent of HIV-positive people were given certain medication to decrease their risk from MTCT (Lloyd-Sherlock, 2019). That same year, 89 percent of HIV-infected newborns were screened within around six weeks after delivery. However, the number of HIV-infected infants born in 2018 remains very high, at 14,000 new-borns.
To meet South Africa’s target of zero transmissions through grandparent transference by 2022, the authorities would try to help women to stick to treatments during nursing, and also during labour and delivery.
Child mortality has also been decreasing but at a far slower pace. Between 1990 and 2015, the preceding national HIV strategy was obtained by minimizing maternal and neonatal mortality besides four different, from 150 fatalities per approximately 1 to 38 losses per 100,000. These objectives, nonetheless, were not fulfilled; the maternal death rate has been estimated to be 119 / 112,546 in 2015 or 117 in the year 2017.
Condom Distribution and its Use
The National AIDS Corporation of South African sought to increase the amount of oral contraception supplied yearly to 850 million between 2000 in some of the current “NSP”. The woman of south Africa organized condom campaign is likewise one of several largest and most followed recognized in the world, having supplied over 28 million emergency contraception in 2016 (Mlatsheni & Ranchhod, 2017). The National AIDS Authority of South Africa intends to raise this figure to 1.6 billion by 2022.
In terms of condom usage, according to the 2017 health Promotion of South Africa prevalence survey, about 56 percent of individuals (ages of 15 to 64) who seemed to have two or more sensual experiences in the last year who used contraception the night before they performed sexual acts. Male and females aged 25 to 49 used condoms at almost the same rate, within about 53%. Among many young individuals (ages 15 to 24), 68 percent of young males with many partners and 47 percent of young women have experienced using a condom that previously they had intercourse with. In comparison, just 33% of older individuals (ages of 50 to 64) with several partners employed condoms.
There are still challenges in maintaining that all condom organizations can serve all communities, particularly including those at increased risk of HIV (Quaife et al. 2018). Condom administration will be expanded under the new approach, with condoms being made accessible in non-traditional locations also including hair salons, gas stations, stores, motels, parking facilities, and brothels, along with community colleges and non-traditional assisted living facilities.
Voluntary Medical Male Circumcision (VMMC)
As per studies published in Sub-Saharan Africa in 2010, Medicaid provides health male genital mutilation (VMMC) can lower the risk incidence white woman Disease transmission besides up to 60%. This prompted the Nigerian Government to launch a nationwide VMMC activity with the goal of attaining 80 percent of “HIV-negative males”.
This aim, however, was not met. In 2017, it was projected that around 32% of young males (ages 15 to 64) have been surgically circumcised. The majority of procedures performed have been performed on young males (ages 15 to 24), having 43 percent receiving VMMC (Vearey et al. 2017). Despite the fact that it is off-target, South Africa continues to expand the incidence of procedures performed. In 2018, about 572,000 informed consent processes were done, up from “485,500” in the year 2015.
Pre-exposure Prophylaxis (PrEP)
South Africa would become the first-ever government in Comment section Africa that has completely approved PrEP in “December 2015”.
In 2019, everything was predicted that amongst 23,000 and 24,000 persons in South Africa would utilize PrEP in actual and upcoming initiatives. The 2017-2022 National Framework plans to increase this to include 85,858 persons from some of the most vulnerable groups receiving PrEP by 2022 (Zizzamia, 2020). An early study of PrEP was undertaken between many “South African women” throughout the year 2015.
HIV Education
Regardless of the extensive risk of complications, numerous people in the younger generation lack a full understanding of the possible prevention methods of HIV. According to a 2019 paper based on research provided by South Africa’s recent National HIV Conduct, and National Surveys, just 11% of younger generations interviewed had complete and correct awareness of HIV, while 25% of the participants had 75 percent knowledge consistency. Young individuals who were jobless or lived in urban and underdeveloped areas were least qualified to be aware of HIV, those that were sexually mature were more HIV-aware than those who weren’t.
In the year 2016, just 5% of schools around The Country provided sexual health learnings, still, again the administration has promised to raise something to 50% in highly endemic regions over the next consecutive five years.
High achievement gaps, a lack of professional preparation, and reluctance in educational institutes due to perceiving the emotional nature of the research topic are all impediments to providing extensive proper “sex education”.
HIV Awareness
Love Life was founded in the year of 1999 and is well known for such ‘ABC’ billboard advertisement, which encouraged ‘abstinence, faithfulness, and condoms’ during the initial periods of the pandemic. Nonetheless, the organization has subsequently shifted its focus to addressing the socioeconomic and environmental determinants of HIV affecting young people, such as discrimination and lack of opportunity. love Life supports young people’s livelihood opportunities using a variety of media channels, including broadcast television. In 2017, love Life’s radio programs addressed over one million individuals worldwide. Furthermore, love Life has participated in over 2,700 schools, directly impacting over 320,000 younger generations.
South Africa’s availability of Antiretroviral Treatment (ART)
South Africa boasts the world’s biggest Education program. Throughout 2018, UNAIDS stated that 4.8 million persons in South Africa started receiving medical treatment. This translates to 62 percent of HIV-positive persons in the nation.
The amount of people available for treatments has more than doubled in recent decades, rising from 3.39 billion U.S. dollars to 9 million in 2018.
Many people are afraid that the rapid expansion of ART will indeed end up damaging institutions and services, lowering the standard of patient healthcare. However, research shows that the increased availability of ART now has no meaningful effect on health outcomes, whether it be in numbers of Ventilator fatalities or illnesses.
Other difficulties with therapy provision, however, have been raised in studies. They discovered that teenagers are more likely to begin ART during advanced adulthood than at a subsequent phase of infection, and have had nearly twice the death rate as females. In the year 2018, 65 percent of Chronic HCV women sought medical attention, compared with 37 percent of HIV-positive males. This emphasizes the need to include males in laboratory testing. In terms of antimicrobial therapy, there’s little to no variation between men and females. In the year 2018, 87 percent of “HIV-positive patients” on medication were word of mouth repressed. Unfortunately, because of a dearth of males checking for HIV, just 47 percent of children or 58 percent of HIV – positive Women are contained.
Continuation in daycare for HIV-positive children is of special importance. Despite surprisingly solid PMTCT attendance and early baby diagnosis, many HIV-positive infants are admitted to treatment late and have low viral suppression rates.
The increased frequency of substance HIV is related to issues of adherence. An investigation of HIV medication resistance in persons who had never been on the application may show that recurrence was less than around 5% until 2009 when it started to increase and peaked at 11.9 percent within the year 2015. The findings back up the Colombian authority’s policy in the year 2017 in order to switch from a typical first-line Portfolio assessment to a Helps control fixed dosage combination, which has been shown to cause fewer adverse effects. It does, however, underline the necessity of a broader attempt to thwart the creation and spread of the substance HIV.
South Africa’s Future of HIV
South Africa also made remarkable growth in coping with its HIV pandemic in current history, and it recently boasts the globe’s largest HIV rehabilitation program. In addition, these programs are now primarily sponsored through South African resources.
HIV prevention efforts are having difficulty larger effects on the process of grandparent transmissions, which is declining substantially. Overall, new infections related to HIV have decreased by percent there in the previous decade, though there are far too many. A dearth of information is impeding HIV prevention measures in particular demographic groups, including adolescent females, furthermore, the imprisonment of vulnerable populations such as sexual violence, as well as persistent gender imbalance. While the relatively brief finance for South Africa’s HIV pandemic is guaranteed, the judiciary must regard additional choices in order to continue and grow its progress.
Reference List
Journals
Amuche, N. J., Emmanuel, E. I., & Innocent, N. E. (2017). HIV/AIDS in sub-Saharan Africa: current status, challenges and prospects. Retrieved from “http://196.43.165.48/bitstream/handle/123456789/460/Emmanuel.pdf?sequence=1&isAllowed=y” Retrieved on 30/10/2021
Chisale, S. S. (2018). Domestic abuse in marriage and self-silencing: Pastoral care in a context of self-silencing. HTS: Theological Studies, 74(2), 1-8. Retrieved from “http://www.scielo.org.za/pdf/hts/v74n2/06.pdf” Retrieved on 30/10/2021
De Wet, N., Amoo, E. O., & Odimegwu, C. O. (2018). Teenage pregnancy in South Africa: Where are the young men involved?. South African Journal of Child Health, 2018(1), s44-s50.Retrieved from “https://journals.co.za/doi/pdf/10.7196/SAJCH.2018.v12i2.1523” Retrieved on 30/10/2021
Dreyer, G. (2018). Clinical implications of the interaction between HPV and HIV infections. Best practice & research Clinical obstetrics & gynaecology, 47, 95-106. Retrieved from “https://repository.up.ac.za/bitstream/handle/2263/62974/Dreyer_Clinical_2018.pdf?sequence=1” Retrieved on 30/10/2021
Du Toit, E., Jordaan, E., Niehaus, D., Koen, L., & Leppanen, J. (2018). Risk factors for unplanned pregnancy in women with mental illness living in a developing country. Archives of women’s mental health, 21(3), 323-331. Retrieved from “https://trepo.tuni.fi/bitstream/handle/10024/103493/risk_factors_for_unplanned_2018.pdf?sequence=1&isAllowed=y” Retrieved on 30/10/2021
Huysamen, M., & Boonzaier, F. (2018). “Out of Africa”: Racist discourse in men’s talk on sex work. Psychology in Society, 57, 58-80.Retrieved from “https://e-space.mmu.ac.uk/624378/1/huysamen-boonzaier%20PINS%20%281%29.pdf” Retrieved on 30/10/2021
Jefferis, T. C., & Theron, L. C. (2017). Promoting resilience among Sesotho-speaking adolescent girls: Lessons for South African teachers. South African Journal of Education, 37(3), 1-11.Retrieved from “file:///C:/Users/User/Downloads/160872-Article%20Text-417212-1-10-20170911.pdf” Retrieved on 30/10/2021
Karim, Q. A., Baxter, C., & Birx, D. (2017). Prevention of HIV in adolescent girls and young women: key to an AIDS-free generation. JAIDS Journal of Acquired Immune Deficiency Syndromes, 75, S17-S26. Retrieved from “https://ukzn-dspace.ukzn.ac.za/bitstream/handle/10413/15136/Abdool_Karim_Quarraisha_2017.pdf?sequence=1&isAllowed=y” Retrieved on 30/10/2021
Lloyd-Sherlock, P. (2019). Long-term care for older people in South Africa: The enduring legacies of apartheid and HIV/AIDS. Journal of Social Policy, 48(1), 147-167. Retrieved from “https://ueaeprints.uea.ac.uk/id/eprint/67040/1/Accepted_manuscript.pdf” Retrieved on 30/10/2021
Mlatsheni, C., & Ranchhod, V. (2017). Youth labour market dynamics in South Africa: Evidence from NIDS 1-2-3. SALDRU, University of Cape Town. Retrieved from “http://www.redi3x3.org/sites/default/files/Mlatsheni%20&%20Ranchhod%202017%20REDI3x3%20Working%20Paper%2039%20Youth%20labour%20market%20dynamics.pdf” Retrieved on 30/10/2021 Njwambe, A., Cocks, M., & Vetter, S. (2019). Ekhayeni: Rural–urban migration, belonging and landscapes of home in South Africa. Journal of Southern African Studies, 45(2), 413-431. Retrieved from “https://www.ru.ac.za/media/rhodesuniversity/content/anthropology/documents/publications/Journal_SAS_PDF.pdf” Retrieved on 30/10/2021 (Njwambe et al. 2019)
Quaife, M., Eakle, R., Cabrera Escobar, M. A., Vickerman, P., Kilbourne-Brook, M., Mvundura, M., … & Terris-Prestholt, F. (2018). Divergent preferences for HIV prevention: a discrete choice experiment for multipurpose HIV prevention products in South Africa. Medical decision making, 38(1), 120-133. Retrieved from “https://researchonline.lshtm.ac.uk/id/eprint/4328565/1/Divergent%20Preferences%20for%20HIV_GREEN%20AAM.pdf” Retrieved on 30/10/2021
Vearey, J. O., Modisenyane, M., & Hunter-Adams, J. (2017). Towards a migration-aware health system in South Africa: a strategic opportunity to address health inequity. South African health review, 2017(1), 89-98. Retrieved from “https://journals.co.za/doi/pdf/10.10520/EJC-c80eeea50” Retrieved on 30/10/2021
Zizzamia, R. (2020). Is employment a panacea for poverty? A mixed-methods investigation of employment decisions in South Africa. World Development, 130, 104938. Retrieved from “https://www.wider.unu.edu/sites/default/files/Events/PDF/Slides/TransEconConf2019-Zizzamia-Rocco.pdf” Retrieved on 30/10/2021
………………………………………………………………………………………………………………………..
Know more about UniqueSubmission’s other writing services:

